BMI, Mortality & Health
There was a lot of attention in the press last week about a new report in the Journal of the American Medical Association (JAMA) showing that BMIs in the “overweight” category (25-30) are associated with lower overall mortality rates. This was accompanied by editorial comments about the need for people to calm down about the fact that U.S. in specific and the world in general is getting fatter. Before taking a deeper dive into the BMI vs. mortality argument here is a link to a post on BMI, and recent overweight/obesity trends in the U.S.
What is the relationship between BMI and mortality?
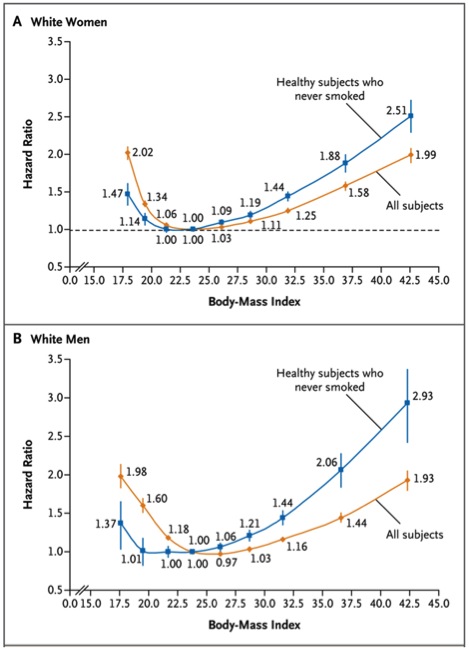
The figure below is from a study of almost 1.5 million whites between the ages of 19 and 84 with a median age of 58. This study has a couple of advantages over the JAMA study especially because it was prospective as opposed to a meta-analysis of prior studies. However, it is restricted to only one racial group. The study also shows that the relationship between mortality and BMI does not really “take off” until people get into the obese (BMI > 30) range. However it is not as reassuring as the JAMA study and mortality does start to creep up in the overweight (BMI 25-30) range. The study concludes that:
“In this large, pooled analysis of prospective studies, both overweight and obesity (and possibly underweight) were associated with increased all-cause mortality in analyses restricted to participants who never smoked and did not have diagnosed cancer or heart disease. Thus, analyses of this subgroup should be minimally confounded by smoking or prevalent illness. The associations were strongest among participants whose BMI was ascertained before the age of 50 years. The lowest all-cause mortality was generally observed in the BMI range of 20.0 to 24.9. Longer follow-up attenuated the associations with lower BMI levels.”
BMI Caveats
The small increases in mortality for the overweight and mildly obese are somewhat reassuring; but the whole relationship between BMI and health is tricky. There are high BMI people who have a lot of muscle mass and not much body fat, and there are low BMI people with a lot of fat who have poor health and increased mortality. This has been termed normal weight obesity, and suggests that low muscle mass can also be a problem. Low muscle mass might also explain some of the mortality issues in people with very low BMIs (<20). There are also high BMI people with plenty of body fat who have normal cholesterol and glucose who are “metabolically healthy”. Thus, there are several patterns of body composition and BMI does is not that predictive on an individual basis. In general abdominal obesity tends to be a bigger problem than fat other places. Here is a link to a Wiki site on abdominal obesity that is informative. Finally, exercise can also modify the relationships between BMI and metabolic health in people in the overweight and obese categories. This is the whole “fit vs. fat debate”.
Mortality vs. Health?
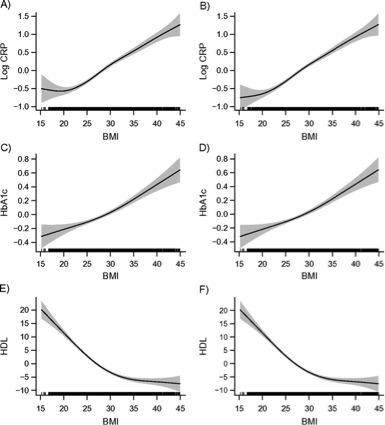
The BMI mortality data does not tell us much about overweight/obesity and health, and this data is hard to come by. However, there is good evidence that so-called biomarkers of disease risk show a more linear vs. U-shaped relationship between BMI and the marker of interest than between BMI and mortality. The figure below shows this for men with data from a large national survey. CRP is a marker of inflammation related to heart disease risk, HBA1c is a marker related to diabetes, and HDL is so-called “good” cholesterol. The panels on the left were statistically adjusted for age and the panels on the right for age and smoking. In the long run the increased risk factors associated with higher BMIs will likely translate into poorer overall health for many people. The authors conclude that:
”These findings imply that obesity researchers should exercise caution when interpreting mortality findings in broader health terms. From a public health perspective, the findings suggest that even moderate levels of overweight may indicate worse health risk profiles than lower body weights, with potentially important implications for chronic disease and health-related quality of life……”
Summary
The relationships between BMI, mortality and health are complicated. Based on the data above we probably should take the “don’t worry” interpretation of the findings in the JAMA paper promoted in the mass media with more than a grain of salt. We also need to think about overweight and obesity using more sophisticated measures of body composition, and a one size fits all BMI based approach to these issues leaves a lot to be desired. The data from the “normal weight obese” and “fit vs. fat” studies along with the very low BMI subgroups in the big population studies suggest that the role of active muscle mass in our overall health is underappreciated. Finally, people tend to gain weight over the years and many of the overweight of today are likely to be the obese of tomorrow.
This entry was posted on Monday, January 7th, 2013 at 6:00 am and is filed under Current Events, Research and Health. You can follow any responses to this entry through the RSS 2.0 feed. You can leave a response, or trackback from your own site.