Archive for November, 2012
More Thoughts About Taxing Unhealthy Behavior
Depending on who you believe any long term solution to the fiscal issues confronting the United States will include revenue increases of 800 billion to 1.6 trillion dollars over the next 10 years. From what I can tell almost all of the discussion about how to raise that revenue focuses on what the well-off will pay. Will their income tax rates be higher, will their deductions be lower, and will the tax code be revamped so that things like capital gains are taxed at a higher rate? As someone interested in public health it seems to me that the revenue, and more importantly behavioral changes, associated with sin taxes should be considered in this debate.
- The Congressional Budget Office estimates that nearly 80 billion dollars could be generated over the next 10 years by increasing the tobacco tax by about 50 cents per pack.
- Obesity researchers and economists from Yale and the University of Illinois Chicago have modeled the effects of a 1 cent per ounce tax on sugary beverages and estimated that nearly 20 billion dollars per year could be generated (200 billion over 10 years).
- The alcohol tax as a percentage of the total cost of various forms of alcoholic beverages is much lower than it was in 1980. If the alcohol tax was 30% of the pretax value of the beverage (it is currently about 10%), a study by the Cato institute estimated that federal revenues would increase by 25 billion dollars per year (250 billion over 10 years)
- Demark recently repealed their so-called fat tax. It was generating about 200 million per year in taxes on high fat foods for the Danes. Extrapolate that to the U.S. which has about 60 times the population of Denmark and you get about 12 billion in revenue per year or 120 billion over 10 years.
All of this adds up to about 650 billion dollars of increased revenue over ten years. Additionally, there is pretty good evidence that smoking rates, health problems associated with excessive drinking, and perhaps even obesity rates might fall if these taxes were enacted. For example a 10% rise in cigarette prices typically reduces consumption by 4%. The sugary beverage tax is estimated to reduce consumption by about 24%, and the alcohol tax is estimated to reduce consumption on the order of 10%. These behavioral changes would likely have positive effects on health care spending over time. There are also economic arguments about improved productivity and increased spending in other parts of the economy that would flow from things like less smoking and drinking.
One of the major arguments against sin taxes is that they fall disproportionately on the poor. However, the counter argument is that the positive behavioral changes associated with these taxes would probably disproportionately benefit the poor in terms of improved health over time and more money to spend on other things. This is especially important because policies that promote positive behavioral health changes in the poor have been difficult to implement and results have been marginal in many cases.
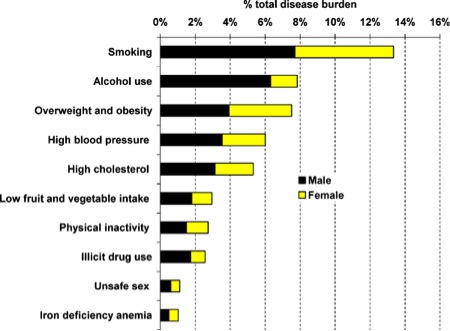
The figure below is from an article on health disparities in 8 socioeconomic groups in the U.S. and shows the role of common behavioral factors in disease burden (for the record I would argue that they grossly underestimated the effects of physical inactivity). These factors are typically higher in the socioeconomic and racial groups with the worst overall health and lowest life expectancy. Increased taxes on tobacco, alcohol and foods contributing to obesity would clearly help reduce the burden from the top four or five causes.
As the article notes:
“Disparities in mortality across the eight Americas, each consisting of millions or tens of millions of Americans, are enormous by all international standards. The observed disparities in life expectancy cannot be explained by race, income, or basic health-care access and utilization alone. Because policies aimed at reducing fundamental socioeconomic inequalities are currently practically absent in the US, health disparities will have to be at least partly addressed through public health strategies that reduce risk factors for chronic diseases and injuries.”
That having been said, I would argue that sin taxes should be attractive to liberals concerned about racial and socioeconomic disparities for statistics like life expectancy and other measures of overall health.
Sin taxes should also be attractive to conservatives who typically espouse a preference for policies that promote personal responsibility. Sin taxes would also help address the current conservative narrative about makers and takers because the increased taxes would tend to fall hardest on states that receive excess federal funds relative to the taxes they pay…..what might be described as “taker” states.
The changes in tax policy that will be made in the coming years have the chance to make things fairer, simpler, more transparent, and perhaps spur economic growth. The ideas outlined above have the added advantage of improving public health, raising revenue, and perhaps driving health care costs down in the longer run. Sin taxes also have the opportunity to address both liberal and conservative policy goals, so shouldn’t they be part of any solution designed to put our financial house in order?
Taxing Unhealthy Behaviors?
There has been a lot of discussion about things like soda taxes to reduce unhealthy behaviors and address the obesity and diabetes epidemic. The idea is that as prices rise, sugary drink consumption will fall and this will have an impact on obesity and diabetes and ultimately reduce some of the upward pressure on health care costs. Along these lines, Denmark implemented a “fat tax” for high fat food items a few years ago but recently reversed the tax for a number of reasons. Importantly, the fat tax in Denmark was not around long enough to determine if it would have any impact on public health. By contrast it is pretty clear that cigarette taxes have contributed to reductions in smoking rates.
Another idea out there is to ask people to pay differing health insurance premiums for what might be called “behavioral” risk factors that are subject to personal choice and changes in behavior. For example, smokers would pay more for their health insurance than non-smokers. The question is how far to take this approach. In some insurance plans there is a move to charge people more for obesity, high cholesterol, hypertension, and diabetes (this would be in addition to higher charges for smokers). The plan would then lower rates or offer rebates as people with “controllable” risk factors addressed their issues and got “their numbers” under control. In other words, if they lost weight, took their blood pressure, cholesterol and/or diabetes medication etc., their costs would go down. The plans are controversial but there is at least some evidence that they work. In the long run this should improve the health of plan members and reduce health care spending over time. For example Safeway reported:
“…the proportion of employees classified as obese declined by five percentage points, while the proportion who were overweight declined by one percentage point. Meanwhile, 40 percent of workers and spouses who failed the blood pressure test in 2008 passed in 2009, 30 percent of former smokers registered as tobacco-free, and 17 percent who failed the cholesterol test in 2008 passed in 2009.”
Absent in the discussion is rating people based on their physical fitness. As an exercise advocate this makes sense to me because exercise is a powerful modifier of other health risk factors.
My take is that a large fraction (estimates are in the 60-90% range) of our health and the diseases we get have major behavioral components. We also know that only a limited number of people follow key health guidelines and practice what might be described as personalized preventive medicine. Should those of us who do follow the guidelines subsidize insurance premiums for those who don’t? That having been said, I think insurance plans that reward personal responsibility are essential to improve public health and reduce health care expenditures –a potential win-win for us all. Premiums schemes that encourage personal responsibility are probably only one part of a comprehensive plan to address lifestyle related diseases, but it seems to me the more messages we send people about the importance of personal responsibility for their own health the better.
Thanksgiving and the Case for Optimism!
This post will go up a few days before Thanksgiving and I want to use it to make the case for optimism about the future. The yapping during the election, the lingering financial crisis, government debt, unemployment, the income gap, natural disasters, global warming, concerns about healthcare and turmoil in the Middle East can make almost anyone pessimistic about the future. If the facts of the day don’t make you a pessimist, the 24 hour news cycle amplifies all of the craziness in a way that challenges the most hard core optimist. So, why I am I an optimist?
First, let’s take a little bit longer view. Think of the “unsolvable” problems confronting the country in say 1968 or 1969:
- The Berlin Wall.
- The Soviet Union invaded Czechoslovakia to suppress a movement calling for minimal levels of free expression.
- George Wallace, an avowed racist, ran for President and got 13.5% percent of the vote.
- Career choices available to women were extremely limited, and opportunities for women and girls to participate in things like competitive sports were minimal.
- Rivers like the Cuyahoga near Cleveland were so polluted they sometimes caught on fire.
- China and India were economic basket cases.
- North Vietnam invaded South Vietnam during Tet.
- Places like Tucson (where I grew up) were surrounded by intercontinental ballistic missile silos. Air raid sirens were tested at regular intervals in case we needed to be warned of an impending nuclear attack.
- The Red Sox had still not won the World Series after trading Babe Ruth to the Yankees in 1918 – the so-called Curse of the Bambino.
I can go on and on with the list, but hopefully you get the message – the list of unsolvable problems changes, and can change pretty fast. People in their 50’s or older who read this will remember many of these “unsolvable” problems, and I would argue that remarkable progress has been made on all of them in ways that were unimaginable or even inconceivable in 1968. The Berlin Wall is down, the Soviet Union is no more, many parts of the environment have been cleaned up, China and India have vibrant economies, and women do all sorts of things including running marathons. The missile silos around Tucson are gone except for one that serves as a museum (visit if you get the chance). However you feel about Barack Obama and the state of racial issues in the U.S., his election and reelection was inconceivable in 1968. Vietnam and the U.S. are now major trading partners. Finally, the Red Sox won the World Series in 2004, proving nothing is impossible.
Don’t believe all the yapping about how bad things are in healthcare and medicine either. For example, when I started medical school in the early 1980s, we watched people have heart attacks, gave them primitive drugs, and hoped they survived. With aggressive treatment many heart attacks are now prevented or stopped in progress and people go on to live long productive lives. Tiny premature babies in the ICU have gone from not surviving at all, to surviving with multiple complications, to routinely surviving with minimal or no complications. I could make a list of 100 or more ways things have gotten not only better but dramatically better in healthcare and medicine.
I would also argue that making sure everyone gets high quality care is a “better problem to have” than the problems associated with having nothing to offer. The same reasoning applies to the U.S. budget and political process. A lot of the current challenges ultimately flow from our aging population. It seems to me that this is a much better problem to have than trying to figure out what to do with a population dying young. Trust me plagues and pestilence are no fun. For the first time in history many young people know all four of their grandparents, what a wonderful problem to have.
In a number of posts over the last few months I have talked about the twin problems of physical inactivity and obesity. Problems flowing from the fact that humans can produce food and labor saving technology in amounts, ways, and varieties that seemed like science fiction only a few generations ago. Like smoking and traffic safety, inactivity and obesity will be solvable and never underestimate how hard life was on a family farm in say 1900. I would rather be trying to figure out how to get people to be more active and eat a bit better than trying to figure out how to get them enough food.
Look again at the 1968 list at the start of the post and compare it to your current favorite problem list and ask yourself two questions:
- How many of the problems on your 2012 list are a consequence of a long term success? In other words we have a “better problem” now like a lot of grandparents around, or global economic competition vs. nuclear confrontation.
- How many of the unsolvable problems on your 2012 list will be there in 40 plus years? Who can predict, but I bet not many.
Finally, humans are incredibly creative and resilient and never underestimate our collective ability to make things better. Optimism is also good for your health, a better way to live and learnable. So, on this Thanksgiving let’s be thankful for the big problems facing our country and the world because they are much better problems to have than the previous big problems. More importantly, they are nothing more than solutions waiting to happen.
Happy Thanksgiving, and the Dr. in me can’t resist reminding everyone to get some exercise, drive carefully, and wear your seat belts!
Aging: Just the Facts
A couple of posts ago I showed you a pie chart of what the US Federal Government spends money on and more than 50% of the total goes to Social Security and Medicare — people who are mostly over 65. This means that our aging population is driving much of the pressure on the budget and will be central to the debate about spending and taxes that continues now that the election is over. That having been said, I think it is essential for us all to have some appreciation of why aging is going to be such a big challenge. The chart below comes from something on the history of Social Security and shows how many people made it to 65 and how long they lived on average after they made it to 65. It starts in 1940 and ends in 1990.
| Percentage of Population Surviving from Age 21 to Age 65 | Average Remaining Life Expectancy for Those Surviving to Age 65 | |||
| Male | Female | Male | Female | |
| 1940 1950 1960 1970 1980 1990 |
53.9 56.2 60.1 63.7 67.8 72.3 |
60.6 65.5 71.3 76.9 80.9 83.6 |
12.7 13.1 13.2 13.8 14.6 15.3 |
14.7 16.2 17.4 18.6 19.1 19.6 |
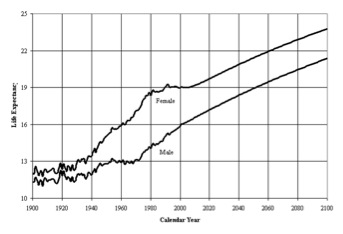
When you update the data in this chart for 2010, it turns out that about 84% of men and 89% of women now make it to 65. The next figure shows that people live even longer now after they make it to 65. The average man who makes it to 65 lives another 16-17 years and for women it is about 19 years. These numbers are projected to continue to rise for both sexes.
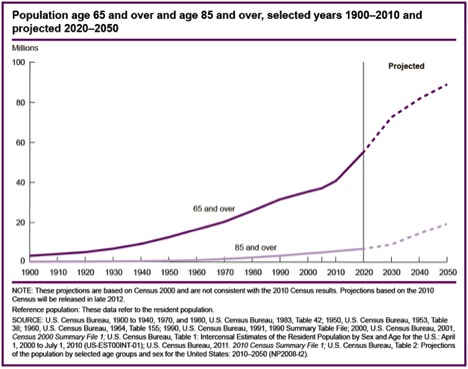
When you put all of this together there is going to be a huge increase in the number of people over age 65 as the Baby Boom generation of roughly 80 million people born between 1946-64 ages. The number of people over age 85 is also going to grow rapidly. The figure below shows those numbers.
I would argue that however we as society ultimately decide to deal with the budgetary challenges ahead via our chaotic political process, we need to do it in a way that fully accounts for the fact that almost all of us will live to be 65 and many of us will make it to 85 or older. I am sure there are people reading this who think we should raise taxes and/or spend less on defense to preserve Social Security and Medicare as they are, others who think benefits should be scaled back, others who think things should be privatized, and others who might do some of all of the above. However, if we are going to do things that both make sense and are politically possible I think we first need a serious dose of demographic reality injected into the discussion. I hope you find the data above useful.
Exercise & Longevity
People exercise for all sorts of reasons including being in better shape to meet the challenges of daily life, weight control, general health, being able to keep up with their kids and grandkids, and participation in competitive activities. But what is the long term payoff in terms of extra years lived or longevity? There is some fascinating new information on the question that comes from a pooled evaluation of a number of large studies conducted over many years by the National Cancer Institute on lifestyle and health in about 650,000 people.
There was enough data in these studies on physical activity and things like BMI to do rigorous statistical analysis on a couple of questions. First the authors had to divide the subjects into groups based on how much physical activity they got per week. The used something called “Met Hours”. A met is a marker of how much oxygen you use per minute at rest and reflects your energy consumption. Brisk walking takes about 3 mets. During peak exercise healthy lean people in their twenties who are untrained max out at about 10-12 mets when they are tested on a treadmill. Without training these peak values fall perhaps 10% per decade starting in our 30s. Elite athletes can achieve max values of 15-20 mets.
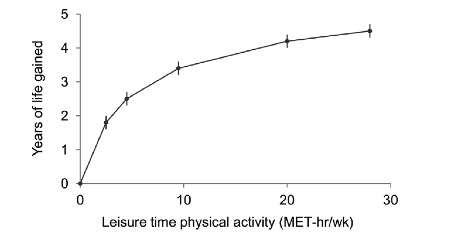
The paper categorized people into six activity groups equal to brisk walking for 0, 1–74, 75–149, 150–299, 300–449, and 450+ minutes per week. In terms of “met hours per week”, these walking categories equal 0, 0.1–3.74, 3.75–7.4, 7.5–14.9, 15.0–22.4, and more than 22.5. Most public health guidelines suggest that 150-299 minutes of moderately vigorous exercise (7.5 to 14.9 met hours) are a key for good health and significantly reduce the risk of things like diabetes and heart disease. The figure below shows the longevity findings.
The authors of the study concluded that:
…..adding even low amounts of leisure time physical activity to one’s daily routine—such as 75 min of walking per week—may increase longevity. This finding may help convince currently inactive persons that a modest physical activity program is “worth it” for health benefits, even if it may not result in weight control. Physical activity above the minimal level—at recommended levels, or even higher—appears to increase longevity even further, with the increase in longevity starting to plateau at approximately 300 min of brisk walking per week. Finally, a lack of leisure time physical activity when combined with obesity is associated with markedly diminished life expectancy. Together, these findings reinforce prevailing public health messages and support them for a range of ages and backgrounds: both a physically active lifestyle and a normal body weight are important for increasing longevity.”
There is not much to add to this except that people who are active also have more disability free years at the end of life. Thus the active live both longer and are more independent as they age with fewer chronic medical problems.
Aging & the Post Election Medicare Debate
In my post just before the election I covered some ideas about what was missing and also some of the inconsistencies in the politics of health care. I also described some of the main factors driving the rise in health care spending including an aging population.
In the next few months both parties will face the so called “Fiscal Cliff” which consists of the expiration of the Bush era tax cuts (e.g. tax increases) and automatic spending cuts that were put in place in 2011. At some level this represents mutual political blackmail by both parties. The thinking goes that the Republicans don’t want the tax increases or cuts in defense spending and the Democrats don’t want cuts in other programs. Thus both parties might actually be incented to reach some sort of compromise and put the long term fiscal health of the country on the right track reminiscent of what Ronald Reagan and Tip O’Neill in the 1980s when they fixed Social Security. If a compromise does emerge, changes in Medicare and Social Security are going to be big topics of the discussion and solution.
I want to show two graphics that I hope will help everyone understand the magnitude of the problem and inform their own thinking about it.
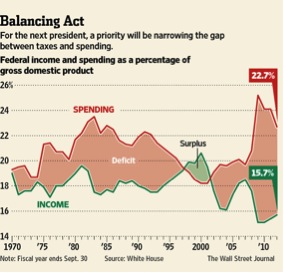
First, both taxes and spending are part of the problem. The figure below is from an excellent pre-election Wall Street Journal article on trends in taxes and spending. It shows that the big yearly deficits recently being run in the U.S. are due to a combination of low taxes and high spending by recent standards.
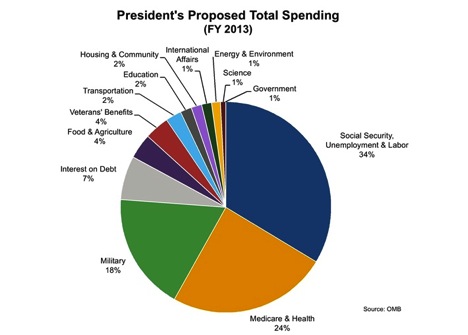
Second, here is a figure of where the Feds spend money as exemplified by the proposed budget for 2013 (it has not been passed yet). The total is just under $3.7 trillion. What is interesting is that a total of 62% is “mandatory” spending on things like Social Security and Medicare. Another 18% or about $65O billion is for the military, and interest on the debt is 7%. With current policies in place the deficit is expected to be about $1 trillion. So even if you cut everything else (Ag programs, medical research, education etc.) to zero you would still have to raise taxes by about $500 billion per year to balance the budget and pay for mandatory programs, the military and interest on the debt. The other long term issue is that most of the mandatory spending is tied to Social Security and Medicare that are for people over 65. Thus these programs are set to grow automatically as the baby boom generation ages and there are more people over 65.
The next link is to a budget calculator game from 2010 that lets you figure out what combination of spending cuts and changes in tax policy you would consider to address the long term budget issues facing the country. I would encourage everyone to play the budget game, we all need to educate ourselves about these issues and understand the choices we face. The goal of the graphics above and the budget game is to give readers the resources to learn more. The simple math I have outlined suggests that changes in Social Security and Medicare spending are coming. More on this in upcoming posts.
Health Care and the Election
Tomorrow is the long awaited election. What strikes me is that most of the discussion about health care has been about the pros and cons of various flavors of what might broadly be called “insurance reform”. Who should be covered? What should be covered? How do we pay for it? How is it regulated? What is the balance between the private sector and government be? Central to all of these concerns are a few big issues:
- In the U.S. we spend a huge fraction (almost 18%) of our GDP on healthcare and yet our public health statistics are not particularly impressive.
- The rise in spending on healthcare in general and Medicare in specific is not sustainable.
- There is a lot of unnecessary spending on procedures and tests – overuse of technology – that probably don’t improve patient outcomes.
- There are a lot of uninsured people, and there is also a lot of political gridlock.
These are all interesting facts, but to me the current political arguments are mostly missing the bus.
Spending vs Public Health Statistics.
The determinants of population health don’t have much to do with the formal healthcare (sick care?) system. I have seen estimates suggesting that 60-80% of population health is about lifestyle, culture and behavioral choices. So, we need to stop confusing what happens when “people go to the Dr.” with public health statistics. As I have pointed out in areas like smoking and traffic safety the U.S. has an excellent track record and many of these strategies could be applied to obesity and inactivity. Also is it fair to compare the U.S. as a whole to smaller more homogenous countries in Europe. When you match various U.S. states with specific countries, things look different. Things are not the same in Athens as they are in Oslo, why should they be the same in Miami and Minneapolis?
Medicare Spending.
I have just a couple of comments on the rise in Medicare spending. At some level doesn’t this represent the problem of “success”? Every developed country in the world and most of the developing countries in the world are undergoing huge shifts in population structure. Humans as a whole are living longer and in 2000, for the first time in world history, there were more people over 60 than under 5. That having been said, I would argue that no matter what we do in terms of “insurance reform” for Medicare in the U.S., it is going to be too little too late in terms of finances unless we promote healthy aging. So again is the problem simply money and resources; or is it really a matter of lifestyle, culture and behavior? There was an interesting article in the NYT magazine on an Island in Greece with a whole bunch of healthy older people, and the story of these islanders is essentially the same old story for healthy aging. Don’t smoke, be active, don’t get fat, stay socially engaged etc.
Overuse of Technology.
The best estimates are that the overuse rate for most things in medicine is about 30%. The question then is how do you turn this around? Some argue that more regulation is needed; some argue that electronic medical records will fix it; some argue that the market can fix it. My guess is that depending on the specifics it will be some of the above, all of the above and none of the above at the same time. However, why not avoid the need for costly interventions by focusing on the root causes of what drive medical costs in the first place? I have said it before, the root causes of what ails us are embedded in our lifestyle, culture and behavior. Why not focus on these issues?
The Uninsured vs. Political Gridlock.
Among the many things I find ironic about the political debate on healthcare reform is the fact that the individual mandate in Obamacare was originally developed by conservative thinkers. Along similar lines ideas about premium support now championed by Paul Ryan (e.g. vouchers) were initially developed by liberal policy wonks. Go figure? How will we ever address the issues of the uninsured, costs, overuse of technology, obesity, inactivity, aging and everything else associated with healthcare if policy ideas are merely ropes in an ongoing political tug of war?
Is there a solution?
I think in the short and medium run we should all do two things:
- Take responsibility for our own health by following key guidelines that I have discussed over and over again in my posts.
- Indicate to the political leadership that focusing on public health initiatives might be a good (and cheap) first step they could all agree on.
If we all did these two things maybe that would give them some time to learn that thoughtful compromise on the other issues will not be fatal and pragmatism is not a disease. Denial can be both.
Exercise and Brain Size
A few weeks ago I pointed out that age associated cognitive impairment and Alzheimer’s disease shared many risk factors with cardiovascular disease. The brain shrinks as it ages and it shrinks faster in people with cognitive impairment and Alzheimer’s disease. There are also other subtle structural changes associated with aging and cognitive decline. A recent paper in the journal Neurology reported on how physical activity affects brain volume in almost 700 people in their 70s who were studied in England.
“A higher level of physical activity was associated with higher fractional anisotropy (a marker of brain structural integrity), larger gray and normal appearing white matter volumes, less atrophy, and lower white matter lesion load. The physical activity associations with atrophy, gray matter, and white matter lesion remained significant after adjustment for covariates, including age, social class, and health status…..”
Conclusions: In this large, narrow-age sample of adults in their 70s, physical activity was associated with less atrophy and white matter lesion. Its role as a potential neuroprotective factor is supported; however, the direction of causation is unclear from this observational study. “
The paper goes on to discuss factors that might be responsible for the positive effects of physical activity on brain size and function. There is evidence that exercise stimulates the growth of new brain cells and improves connections between brain cells, so no major surprises here.
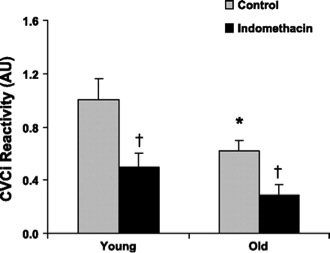
The paper also mentions that exercise may also improve blood flow to the brain. The figure below is from a study done in my lab by Dr. Jill Barnes. It shows using a measurement called CVCi, that the ability of the brain blood vessels to relax and vasodilate (usually a good thing) in response to CO2 is lower in healthy 60 somethings vs 20 somethings. In both age groups a drug called indomethacin reduced the vasodilation in response to CO2. Blood flow at rest was also lower in the older subjects, or as Dr. Barnes put it:
“Young adults demonstrated greater MCAv (index of blood flow) 55 ± 6 vs. 39 ± 5 cm/s and MCAv reactivity 1.67 ± 0.20 vs. 1.09 ± 0.19 cm·s to hypercapnia (CO2) compared with older adults.”
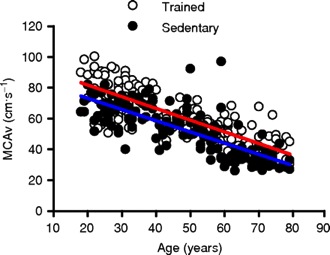
The next figure I want to show you is from a study on aging and brain blood flow in trained and untrained male subjects.
The authors commented that:
This ∼17% difference between trained and sedentary men amounted to an approximate 10 year reduction in MCAv (blood flow) ‘age’ and was robust to between-group differences in BMI and blood pressure. Regular aerobic-endurance exercise is associated with higher MCAv in men aged 18–79 years.
Summary: Exercise and physical activity do good things for your brain as you age. They help you grow new cells and they keep blood flow to the brain high. One idea is that blood flow is higher because the brain remains bigger in those who are active as they age. The other interesting thing to note is the “10 year” anti-aging effects of exercise on blood flow. That number, or perhaps an even higher one, seems to be pretty consistent for the anti-aging effects of exercise on many elements of our physiology.
You are currently browsing the Human Limits blog archives for November, 2012.